Our bodies are made up of trillions of cells that work together to keep us alive. A major challenge in their success is communication between cells in different parts of the body. Our cells have ingenious ways of overcoming this challenge, with exosomes emerging as key players. Exosomes are cell-derived vesicles that can carry cargo in the form of nucleic acids, lipids, or proteins from one cell to another. The sender cell packages cargo into an exosome, which then leaves the cell by being pinched off from the cell membrane. The exosome finds it way to a neighboring cell or into the bloodstream, from which it can be sent throughout the body. The exosome has signs on its surface that determine what cells can receive the cargo, so it only goes to the intended receiver. If a heart cell wants to talk to another heart cell, it puts markers on its exosomes that make them stick to other heart cells. When those exosomes are taken into the receiving cells, their cargo can bring about physiologic changes there.
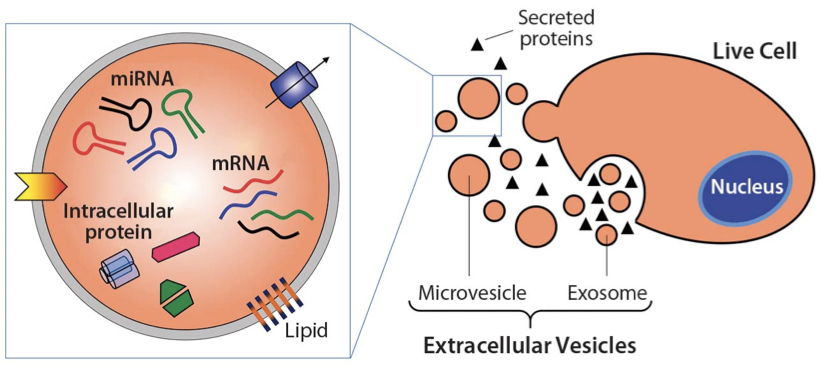
Extracellular vesicles and their cargo. Source: BioProcess International.
Exosomes play a major role not only in our regular physiology but also in disease. One of the fields in which the role of exosomes is being uncovered is cardiovascular disease. For example, heart endothelial cells (cells that line the blood vessels) communicate with heart muscle cells via exosomes that contain microRNA, a kind of molecule that can decrease how many transcripts of a particular set of genes get made in the target cell. This process may play a role in the heart’s response to plaque formation. One can envision the possibility for engineering exosomes so that we can communicate with our bodies to treat or prevent disease. The lab of Dr. Susmita Sahoo at the Icahn School of Medicine at Mount Sinai is interested in doing just that.
Before talking about how Dr. Sahoo’s group is using exosomes in treating heart failure, let’s talk about a specific cause of heart failure: epitranscriptomics. You may or may not have heard of epigenetics, which is the study of heritable, chemical changes to DNA that do not change the sequence of the DNA. Epitranscriptomics is based on the exact same idea, but the change happens at the RNA level. One such epitranscriptomic modification is the addition or removal of methyl groups on adenosines within certain mRNAs in cells.
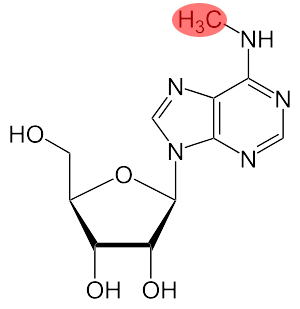
Structure of N6-Methyladenosine (m6A)
Heart muscle cells (cardiomyocytes) usually use electrical signals to interact and pulse in unison with a set rhythm. Work from Dr. Sahoo’s team suggests that decreasing levels of FTO, an enzyme that removes these methyl groups from RNA, leads to arrhythmia, a disturbance in that synchronized pulse. This finding is corroborated by the fact that failing hearts have low levels of FTO and elevated levels of mRNA methylation. Delivering exosomes with extra FTO to these cells might help them maintain healthy levels of FTO and decrease the chance of heart failure; this approach holds tremendous promise for the treatment of heart disease.
Dr. Sahoo’s research on exosomes is not limited to the failing heart. Recent work from her group suggests that a specific type of exosome, known to carry a marker called CD34 on its surface, improves angiogenesis, or formation of new blood vessels. Angiogenesis is a crucial step in healing after an injury. Dr. Sahoo’s group has shown that exosomes are able to improve healing in mice by providing microRNAs important for angiogenesis to cells near the site of injury. This work is not only important in helping patients after an injury, but it also teaches us about fundamental roles of microRNAs in angiogenesis and gene regulation.
We have outlined only some of the work going on in Dr. Sahoo’s lab. You can visit her website or watch her recent ERCC seminar to learn more about exosomes and her research on their role in cardiac medicine.
There are no comments.